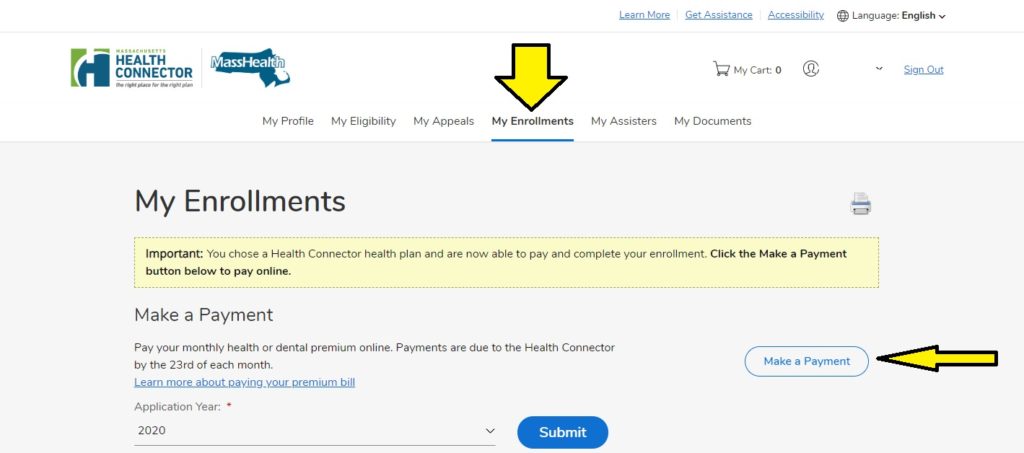
Please call her when she needs to fill out her redetermination paperwork. "As someone who has a family member who's blind, happens to be my mother. "I don't buy for a second that 150 people are going to help the situation," Ferrante said at the hearing. Ann-Margaret Ferrante of Gloucester said she is worried that elderly and disabled people are going to have trouble navigating the redetermination process, regardless of the new hires. There are skeptics about MassHealth's call center hiring.Īfter personal and professional challenges navigating the MassHealth system, state Rep. “But I don't want people to worry right now until they receive that letter, right now what people need to do is to really update the information so that they can receive the letter, and they can take action once they receive the letter.” “After they receive the blue envelope they will have 45 days to respond, and that's when they really need to take action,” she said. “Until they are up for renewal, until they complete the redetermination process, they are going to be covered by MassHealth.”įor those who do not qualify for auto-renewal, Gonzalez said they should update their contact information through MassHealth and be on the lookout for blue envelopes arriving in the mail which contain instructions for redetermination. “The message really is that even though the health insurance landscape is extremely complicated to navigate, Massachusetts has a lot of programs and has a lot of opportunities for people to have access to health insurance,” Gonzalez said. 
Maria Gonzalez, the MassHealth Redetermination Campaign Director at Health Care For All, a nonprofit advocacy group focused on promoting health equity and fair access to medical coverage, said the goal is not to kick anyone off insurance. “There is no need to panic, there are windows built into the redetermination process so that people don't lose coverage immediately,” Cyr said. Julian Cyr, D-Truro, said about half of MassHealth members are expected to be automatically renewed. These calls will take 90 to 120 minutes, "but it's a start" at making the process more accessible, he said.īeginning in May, MassHealth officials will begin publishing a public dashboard that will show where the people who are losing MassHealth coverage live, their demographics, and the reasons behind lost coverage. The agency cut the long MassHealth application by about 75 percent for applicants over 65 years old, Levine said, and next month they will begin allowing seniors to do their applications over the phone. Levine said MassHealth is looking to make the application process easier and remain transparent throughout the redetermination process. The agency is ramping up its workforce across the board, Levine said, including doubling the amount of customer service representatives in call centers to 320, hiring an additional 100 workers to determine eligibility, 80 to 100 temporary employees to process applications, and using grants to scale up the certified application counselor workforce. MassHealth is boosting its workforce to help deal with redetermination of eligibility 
Maura Healey's fiscal 2024 budget proposal, Assistant Secretary for MassHealth Michael Levine said that the public insurance program is preparing for the onslaught of work checking the eligibility of those 2.3 million enrollees, and helping those who no longer qualify transition to other coverage.Īs the state struggles with a labor crunch, MassHealth hopes to double its call center workforce capacity in the next two months to deal with determining eligibility. At a Joint Ways and Means Committee hearing on health care investments in Gov.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
